| 1 |
Liu P, Gao C, Chen H, et al. Receptor-mediated targeted drug delivery systems for treatment of inflammatory bowel disease: Opportunities and emerging strategies[J]. Acta Pharm Sin B, 2021, 11 (9): 2798- 2818.
doi: 10.1016/j.apsb.2020.11.003
|
| 2 |
Ward D, Nyboe Andersen N, Gørtz S, et al. Tumor necrosis factor inhibitors in inflammatory bowel disease and risk of immune mediated inflammatory diseases [J]. Clin Gastroenterol Hepatol, 2024, 22(1): 135-143. e8.
|
| 3 |
Yang Q, Li SS, Ou HB, et al. Exosome-based delivery strategies for tumor therapy: an update on modification, loading, and clinical application[J]. J Nanobiotechnol, 2024, 22 (1): 41.
doi: 10.1186/s12951-024-02298-7
|
| 4 |
Shan YL, Zhang MY, Tao EX, et al. Pharmacokinetic characteristics of mesenchymal stem cells in translational challenges[J]. Signal Transduction Targeted Therapy, 2024, 9 (1): 242.
doi: 10.1038/s41392-024-01936-8
|
| 5 |
Zhang Q, Shan Y, Shen L, et al. Renal remodeling by CXCL10-CXCR3 axis-recruited mesenchymal stem cells and subsequent IL4I1 secretion in lupus nephritis[J]. Signal Transduction Targeted Therapy, 2024, 9 (1): 325.
doi: 10.1038/s41392-024-02018-5
|
| 6 |
Ni Q, Zhen L, Zeng Z, et al. Mesenchymal stromal cells restrain the Th17 cell response via L-amino-acid oxidase within lymph nodes[J]. Cell Death Dis, 2024, 15 (9): 640.
doi: 10.1038/s41419-024-07024-7
|
| 7 |
Eggenhofer E, Benseler V, Kroemer A, et al. Mesenchymal stem cells are short-lived and do not migrate beyond the lungs after intravenous infusion[J]. Frontiers Immunol, 2012, 3, 297.
doi: 10.3389/fimmu.2012.00297
|
| 8 |
Li S, Li W, Wu X, et al. Immune cell-derived extracellular vesicles for precision therapy of inflammatory-related diseases[J]. J Control Release, 2024, 368, 533- 547.
doi: 10.1016/j.jconrel.2024.03.007
|
| 9 |
Kalluri R, Mcandrews KM. The role of extracellular vesicles in cancer[J]. Cell, 2023, 186 (8): 1610- 1626.
doi: 10.1016/j.cell.2023.03.010
|
| 10 |
Buzas EI. The roles of extracellular vesicles in the immune system[J]. Nat Rev Immunol, 2022, 23 (4): 236- 250.
doi: 10.1038/s41577-022-00763-8
|
| 11 |
Kalluri R. The biology and function of extracellular vesicles in immune response and immunity[J]. Immunity, 2024, 57 (8): 1752- 1768.
doi: 10.1016/j.immuni.2024.07.009
|
| 12 |
Das S, Lyon CJ, Hu T. A panorama of extracellular vesicle applications: from biomarker detection to therapeutics[J]. ACS Nano, 2024, 18 (14): 9784- 9797.
doi: 10.1021/acsnano.4c00666
|
| 13 |
Herrmann IK, Wood MJA, Fuhrmann G. Extracellular vesicles as a next-generation drug delivery platform[J]. Nat Nanotechnol, 2021, 16 (7): 748- 759.
doi: 10.1038/s41565-021-00931-2
|
| 14 |
Colombo M, Raposo G, Théry C. Biogenesis, secretion, and intercellular interactions of exosomes and other extracellular vesicles[J]. Ann Rev Cell Develop Biol, 2014, 30 (1): 255- 289.
doi: 10.1146/annurev-cellbio-101512-122326
|
| 15 |
刘苡佳, 刘斌, 胡奎, 等. 干细胞和巨噬细胞来源的外泌体对结肠炎的调控作用及其机制[J]. 实用医学杂志, 2025, 41 (3): 447- 453.
doi: 10.3969/j.issn.1006-5725.2025.03.022
|
| 16 |
Welsh JA, Goberdhan DCI, O'Driscoll L, et al. Minimal information for studies of extracellular vesicles (MISEV2023): From basic to advanced approaches[J]. J Extracel Ves, 2024, 13 (2): e12404.
doi: 10.1002/jev2.12404
|
| 17 |
Théry C, Witwer KW, Aikawa E, et al. Minimal information for studies of extracellular vesicles 2018 (MISEV2018): a position statement of the International Society for Extracellular Vesicles and update of the MISEV2014 guidelines[J]. J Extracel Ves, 2018, 7 (1): 1535750.
doi: 10.1080/20013078.2018.1535750
|
| 18 |
李青, 李博, 陈政升, 等. 团体标准《人多能干细胞来源的小细胞外囊泡》与《人间充质干细胞来源的小细胞外囊泡》解读[J]. 中国研究型医院, 2023, 10 (3): 47- 50.
doi: 10.19450/j.cnki.jcrh.2023.03.010
|
| 19 |
Chen M, Lin S, Zhou C, et al. From conventional to microfluidic: progress in extracellular vesicle separation and individual characterization[J]. Adv Healthc Mater, 2023, 12 (8): e2202437.
doi: 10.1002/adhm.202202437
|
| 20 |
Rupp AK, Rupp C, Keller S, et al. Loss of EpCAM expression in breast cancer derived serum exosomes: Role of proteolytic cleavage[J]. Gynecol Oncol, 2011, 122 (2): 437- 446.
doi: 10.1016/j.ygyno.2011.04.035
|
| 21 |
Ma XX, Peng LW, Zhu XH, et al. Isolation, identification, and challenges of extracellular vesicles: emerging players in clinical applications[J]. Apoptosis, 2024, 30 (1/2): 422- 445.
|
| 22 |
Hass R, Von Der Ohe J, Luo TJ. Human mesenchymal stroma/stem-like cell-derived taxol-loaded EVs/exosomes transfer anti-tumor microRNA signatures and express enhanced SDF-1-mediated tumor tropism[J]. Cell Commu Signal, 2024, 22 (1): 506.
doi: 10.1186/s12964-024-01886-2
|
| 23 |
Eldh M, Lötvall J, Malmhäll C, et al. Importance of RNA isolation methods for analysis of exosomal RNA: Evaluation of different methods[J]. Mol Immunol, 2012, 50 (4): 278- 286.
doi: 10.1016/j.molimm.2012.02.001
|
| 24 |
Xie M, Li CF, She Z, et al. Human umbilical cord mesenchymal stem cells derived extracellular vesicles regulate acquired immune response of lupus mouse in vitro[J]. Scientific Rep, 2022, 12 (1): 13101.
doi: 10.1038/s41598-022-17331-8
|
| 25 |
Zhang B, Lai RC, Sim WK, et al. Topical Application Of Mesenchymal Stem Cell Exosomes Alleviates The Imiquimod Induced Psoriasis-Like Inflammation[J]. Int J Mol Sci, 2021, 22 (2): 720.
doi: 10.3390/ijms22020720
|
| 26 |
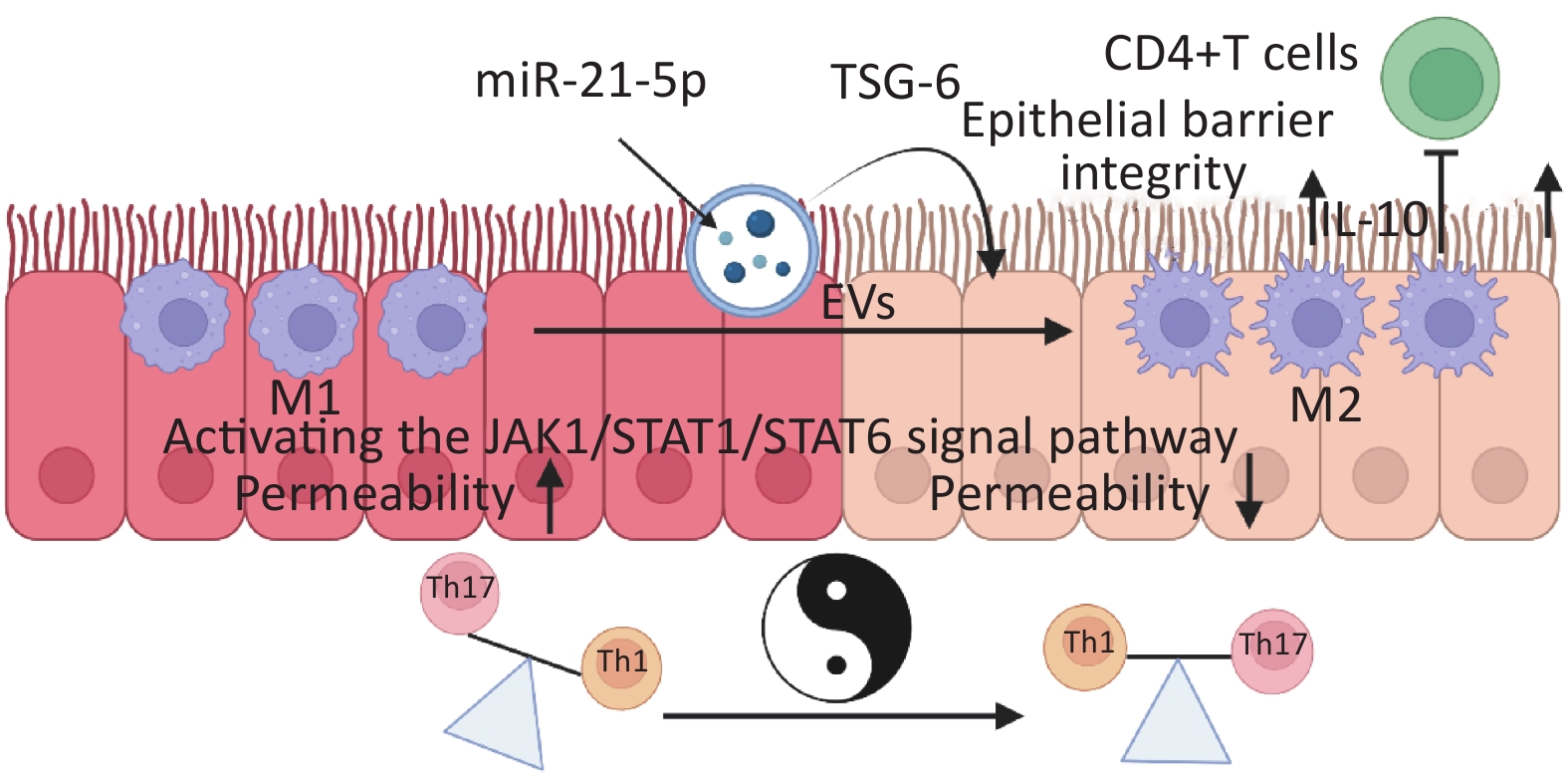
Qian W, Wu E, Chen H, et al. MSCs-exosomes can promote macrophage M2 polarization via exosomal miR-21-5p through Mesenteric injection: a promising way to attenuate murine colitis [J]. J Crohns Colitis, 2024: jjae110.
|
| 27 |
Lee JH, Lötvall J, Cho BS. The anti-inflammatory effects of adipose tissue mesenchymal stem cell exosomes in a mouse model of inflammatory bowel disease[J]. Int J Mol Sci, 2023, 24 (23): 16877.
doi: 10.3390/ijms242316877
|
| 28 |
Zhang K, Guo J, Yan W, et al. Macrophage polarization in inflammatory bowel disease[J]. Cell Commun Signal, 2023, 21 (1): 367.
doi: 10.1186/s12964-023-01386-9
|
| 29 |
Cao L, Xu HX, Wang G, et al. Extracellular vesicles derived from bone marrow mesenchymal stem cells attenuate dextran sodium sulfate-induced ulcerative colitis by promoting M2 macrophage polarization[J]. Int Immunopharmacol, 2019, 72, 264- 274.
doi: 10.1016/j.intimp.2019.04.020
|
| 30 |
Yang S, Liang X, Song J, et al. A novel therapeutic approach for inflammatory bowel disease by exosomes derived from human umbilical cord mesenchymal stem cells to repair intestinal barrier via TSG-6[J]. Stem Cell Res Ther, 2021, 12 (1): 315.
doi: 10.1186/s13287-021-02404-8
|
| 31 |
Liu H, Liang Z, Wang F, et al. Exosomes from mesenchymal stromal cells reduce murine colonic inflammation via a macrophage-dependent mechanism[J]. JCI Insight, 2019, 4 (24): e131273.
doi: 10.1172/jci.insight.131273
|
| 32 |
Geremia A, Biancheri P, Allan P, et al. Innate and adaptive immunity in inflammatory bowel disease[J]. Autoimmu Rev, 2014, 13 (1): 3- 10.
doi: 10.1016/j.autrev.2013.06.004
|
| 33 |
Chen QY, Duan XY, Xu M, et al. BMSC-EVs regulate Th17 cell differentiation in UC via H3K27me3[J]. Mol Immunol, 2020, 118, 191- 200.
doi: 10.1016/j.molimm.2019.12.019
|
| 34 |
Tian J, Zhu QG, Zhang YD, et al. Olfactory ecto-mesenchymal stem cell-derived exosomes ameliorate experimental colitis modulating Th1/Th17 and Treg cell responses[J]. Front Immunol, 2020, 11, 598322.
doi: 10.3389/fimmu.2020.598322
|
| 35 |
Citi S. Intestinal barriers protect against disease[J]. Science, 2018, 359 (6380): 1097- 1098.
doi: 10.1126/science.aat0835
|
| 36 |
Yu H, Yang X, Xiao X, et al. Human adipose mesenchymal stem cell-derived exosomes protect mice from DSS-induced inflammatory bowel disease by promoting intestinal-stem-cell and epithelial regeneration[J]. Aging Dis, 2021, 12 (6): 1423- 1437.
doi: 10.14336/AD.2021.0601
|
| 37 |
Liang X, Li C, Song J, et al. HucMSC-Exo promote mucosal healing in experimental colitis by accelerating intestinal stem cells and epithelium regeneration via Wnt signaling pathway[J]. Int J Nanomed, 2023, 18, 2799- 2818.
doi: 10.2147/IJN.S402179
|
| 38 |
Cai X, ZHang ZY, Yuan JT, et al. hucMSC-derived exosomes attenuate colitis by regulating macrophage pyroptosis via the miR-378a-5p/NLRP3 axis[J]. Stem Cell Res Ther, 2021, 12 (1): 416.
doi: 10.1186/s13287-021-02492-6
|
| 39 |
Heidari N, Abbasi-Kenarsari H, Namaki S, et al. Adipose-derived mesenchymal stem cell-secreted exosome alleviates dextran sulfate sodium-induced acute colitis by Treg cell induction and inflammatory cytokine reduction[J]. J Cell Physiol, 2021, 236 (8): 5906- 5920.
doi: 10.1002/jcp.30275
|
| 40 |
Wei Z, Hang S, Wiredu Ocansey DK, et al. Human umbilical cord mesenchymal stem cells derived exosome shuttling mir-129-5p attenuates inflammatory bowel disease by inhibiting ferroptosis[J]. J Nanobiotechnol, 2023, 21 (1): 188.
doi: 10.1186/s12951-023-01951-x
|
| 41 |
Yang R, Huang H, Cui S, et al. IFN-γ promoted exosomes from mesenchymal stem cells to attenuate colitis via miR-125a and miR-125b[J]. Cell Death Dis, 2020, 11 (7): 603.
doi: 10.1038/s41419-020-02788-0
|
| 42 |
Wong WY, Lee MML, Chan BD, et al. Proteomic profiling of dextran sulfate sodium induced acute ulcerative colitis mice serum exosomes and their immunomodulatory impact on macrophages[J]. Proteomics, 2016, 16 (7): 1131- 1145.
doi: 10.1002/pmic.201500174
|
| 43 |
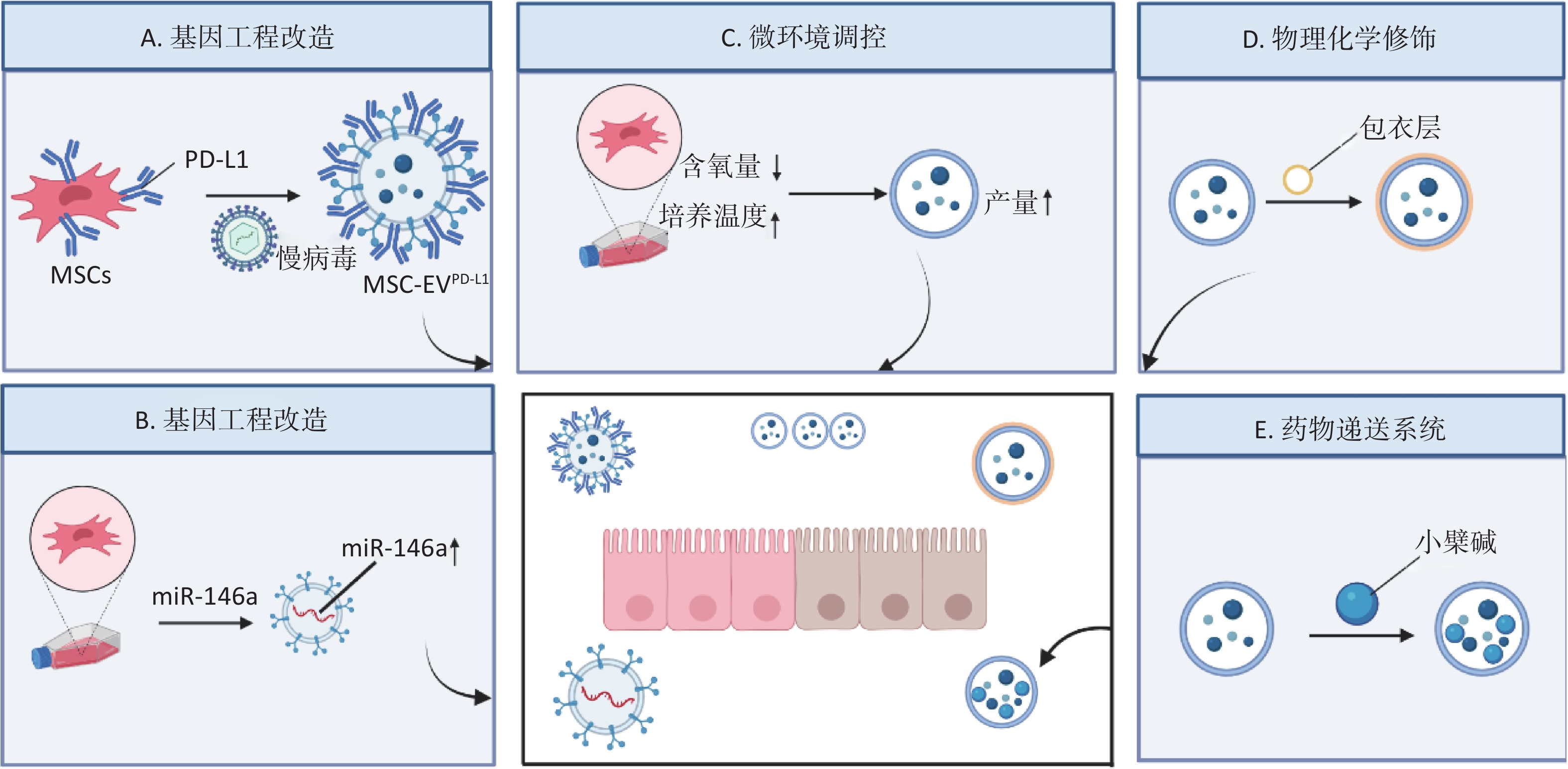
Xu F, Fei Z, Dai H, et al. Mesenchymal stem cell‐derived extracellular vesicles with high PD‐L1 expression for autoimmune diseases treatment[J]. Adv Materials, 2021, 34 (1): e2106265.
|
| 44 |
Nie M, Huang D, Chen G, et al. Bioadhesive microcarriers encapsulated with IL‐27 high expressive MSC extracellular vesicles for inflammatory bowel disease treatment[J]. Advanced Science, 2023, 10 (32): e2303349.
doi: 10.1002/advs.202303349
|
| 45 |
Wu H, Fan H, Shou Z, et al. Extracellular vesicles containing miR-146a attenuate experimental colitis by targeting TRAF6 and IRAK1[J]. Int Immunopharmacol, 2019, 68, 204- 212.
doi: 10.1016/j.intimp.2018.12.043
|
| 46 |
Ambattu LA, Ramesan S, Dekiwadia C, et al. High frequency acoustic cell stimulation promotes exosome generation regulated by a calcium-dependent mechanism[J]. Commun Biol, 2020, 3 (1): 553.
doi: 10.1038/s42003-020-01277-6
|
| 47 |
Tang D, Liu M, Gao S, et al. Thermally engineered MSC-derived extracellular vesicles ameliorate colitis in mice by restoring the imbalanced Th17/Treg cell ratio[J]. Int Immunopharmacoly, 2023, 125, 111077.
doi: 10.1016/j.intimp.2023.111077
|
| 48 |
Qian W, Huang L, Xu Y, et al. Hypoxic ASCs-derived Exosomes attenuate colitis by regulating macrophage polarization via miR-216a-5p/HMGB1 axis[J]. Inflamma Bowel Dis, 2023, 29 (4): 602- 619.
doi: 10.1093/ibd/izac225
|
| 49 |
Deng C, Hu Y, Conceição M, et al. Oral delivery of layer-by-layer coated exosomes for colitis therapy[J]. J Control Rel, 2023, 354, 635- 650.
doi: 10.1016/j.jconrel.2023.01.017
|
| 50 |
Gan J, Sun L, Chen G, et al. Mesenchymal stem cell exosomes encapsulated oral microcapsules for acute colitis treatment[J]. Advanced Healthcare Materials, 2022, 11 (17): e2201105.
doi: 10.1002/adhm.202201105
|
| 51 |
Mofazali P, Atapour M, Nakamura M, et al. Evaluation of layer-by-layer assembly systems for drug delivery and antimicrobial properties in orthopaedic application[J]. Int J Pharmac, 2024, 657, 124148.
doi: 10.1016/j.ijpharm.2024.124148
|
| 52 |
Borges J, Zeng J, Liu XQ, et al. Recent developments in layer‐by‐layer assembly for drug delivery and tissue engineering applications[J]. Advanced Healthcare Materials, 2024, 13 (8): e2302713.
doi: 10.1002/adhm.202302713
|
| 53 |
Barile L, Vassalli G. Exosomes: Therapy delivery tools and biomarkers of diseases[J]. Pharmacol Ther, 2017, 174, 63- 78.
doi: 10.1016/j.pharmthera.2017.02.020
|
| 54 |
Deng C, Hu Y, Conceicao M, et al. Oral delivery of layer-by-layer coated exosomes for colitis therapy[J]. J Control Release, 2023, 354, 635- 650.
doi: 10.1016/j.jconrel.2023.01.017
|
| 55 |
Tang X, Shang Y, Yang H, et al. Targeted delivery of Fc-fused PD-L1 for effective management of acute and chronic colitis[J]. Nat Commu, 2024, 15 (1): 1673.
doi: 10.1038/s41467-024-46025-0
|
| 56 |
Fu YJ, Zhao X, Wang LY, et al. A gas therapy strategy for intestinal flora regulation and colitis treatment by nanogel‐based multistage NO delivery microcapsules[J]. Advanced Materials, 2024, 36 (19): e2309972.
doi: 10.1002/adma.202309972
|
| 57 |
Zhang Y, Ma R, You C, et al. Hyaluronic acid modified oral drug delivery system with mucoadhesiveness and macrophage-targeting for colitis treatment[J]. Carbohydrate Polymers, 2023, 313, 120884.
doi: 10.1016/j.carbpol.2023.120884
|
| 58 |
王心怡, 付淑军, 孟祥骏, 等. 纳米药物递送系统体内命运分析新方法与新技术研究进展[J]. 药学进展, 2024, 48 (10): 747- 760.
doi: 10.20053/j.issn1001-5094.2024.10.004
|
| 59 |
Sun L, Liu H, Ye Y, et al. Smart nanoparticles for cancer therapy[J]. Signal Transduction Targeted Therapy, 2023, 8 (1): 418.
doi: 10.1038/s41392-023-01642-x
|
| 60 |
Zhao S, Di Y, Fan H, et al. Targeted delivery of extracellular vesicles: the mechanisms, techniques and therapeutic applications[J]. Mol Biomed, 2024, 5 (1): 60.
doi: 10.1186/s43556-024-00230-x
|
| 61 |
Deng C, Zhang H, Li Y, et al. Exosomes derived from mesenchymal stem cells containing berberine for ulcerative colitis therapy[J]. J Coll Inter Sci, 2024, 671, 354- 373.
doi: 10.1016/j.jcis.2024.05.162
|
| 62 |
Guo J, Wang F, Hu Y, et al. Exosome-based bone-targeting drug delivery alleviates impaired osteoblastic bone formation and bone loss in inflammatory bowel diseases[J]. Cell Rep Med, 2023, 4 (1): 100881.
doi: 10.1016/j.xcrm.2022.100881
|
| 63 |
Greenberg ZF, Graim KS, He M. Towards artificial intelligence-enabled extracellular vesicle precision drug delivery[J]. Advanced Drug Delivery Reviews, 2023, 199, 114974.
doi: 10.1016/j.addr.2023.114974
|
| 64 |
Nademi Y, Tang T, Uludağ H. Modeling uptake of polyethylenimine/short interfering RNA nanoparticles in breast cancer cells using machine learning[J]. Advanced NanoBiomed Res, 2021, 1 (10): 2000106.
doi: 10.1002/anbr.202000106
|